|
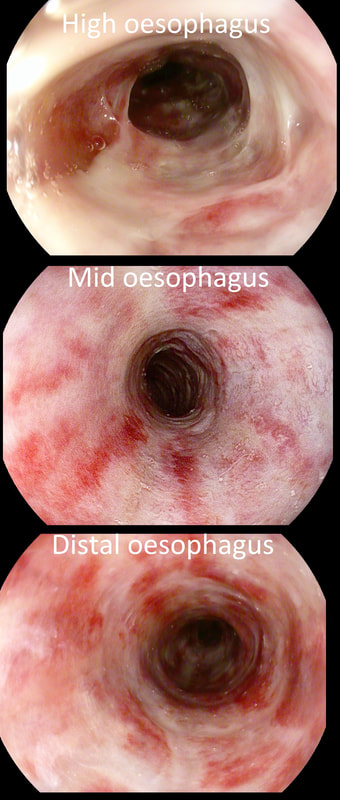
This patient is attending for dilatation of a high oesophageal stricture but there is a surprise. WHAT IS THE CAUSE OF THE STRICTURING?
■ Corrosive ingestion
Yes, a likely cause of 2 high oesophageal strictures
■ Peptic ulceration
In the high oesophagus?!?
■ Lichen planus
Possible but never seen two !
■ Eosinophilic oesophagitis
They are not short and membrane-like!
■ SCC
The mucosa is unremarkable!!!
explanation
The 'surprise finding' is of course that there are TWO strictures some 2-3cm apart in the high oesophagus. All of the above could be the cause, I guess. Of course, the stricture does not look malignant. Eosinophilic oesophagitis gives smoother, long tapering strictures, not short membrane-like strictures like this. Peptic ulceration would be unlikely in the high oesophagus (unless there is a long stretch of Barrett's below). Lichen planus is a possibility but the fact that there are more than one strictures, makes corrosive ingestion the most likely diagnosis. Actually, the patient had been admitted after swallowing a lot of toilet cleaner a few months earlier.
in the images below you can see what her oesophagus looked like after that alkaline burn. I wonder if giving a reducing dose of steroid, like we do after large oesophageal EMR's could have prevented her stricture? This patient was admitted following drinking caustic soda. This was the oesophageal findings a day after admission. WHICH STATEMENT DO YOU AGREE WITH? a) what was the point of the OGD? b) the appearances indicate a likely good outcome c) the appearances indicate that surgery is likely to be required explanation
Older management algorithms of corrosive ingestion usually involve endoscopy (BMC Gastroenterol. 2008;8:31). Unfortunately, endoscopy is unable to accurately predict the depth of intramural necrosis (J Am Coll Surg. 1999;189:508–522). In fact, CT has been shown to be far more reliable in predicting transmural oesophageal necrosis and identify those patients who require surgery (Surg Endosc. 2015;29:1452–1461). In the largest, prospective study to date, from Paris (Ann Surg 2016;264:107-13) , 120 patients admitted with a corrosive injury underwent both a gastroscopy and CT. Ultimately, 24 patients (20%) required an surgery, 28 patients (23%) developed a stricture and 3 patients died. The authors concluded that 'poor predictors' or signs of more severe corrosive injury and a greater risk of perforation included: burns visible inside the mouth, ↑ serum lactate, alanine ↑ aminotransferase and ↑ bilirubin levels or a ↓ in the platelet count below normal range. Rather as expected, CT was found to be far better than endoscopy in identifying patients with full thickness necrosis of either the oesophagus or the stomach. In fact, there was not one single instance when the endoscopy contributed to the decision making! I do worry about scoping these patients, particularly in the early stages because if they 'perforate', you may be open to the accusation, that you actually 'caused' the perforation. You can imagine the scenario. A precious daughter undergoes an emergency gastroscopy following which things take a turn for the worse. Would it be surprising if the family start suspecting that the endoscopy may have had something to do with the deterioration ? Of course, accidental ingestion of corrosives is common problem in children. In children, it has been estimated that between 7% and 20% develop oesophageal strictures after corrosive ingestion (J Laryngol Otol 1996; 110:1041–5). This figure is lower than for adults, perhaps because children will end up swallowing less corrosive than adults. Unfortunately, in both children and adults, the strictures are often multiple and are usually very fibrous requiring multiple dilatations. An UK regional audit reported an overall perforation rate of 2.6% for oesophageal dilatation with a mortality of 1% . The risk of perforation was lower when dilating benign strictures (1.1% with a mortality of 0.5%) than malignant strictures (6.4% with a mortality of 2.3%) or achalasia (usually 3–4% with a mortality rate <1%). Oesophageal dilatation is most risky in the elderly with reduced tissue strength or when the endoscopist is inexperienced and when strictures are complex, particularly when using weighted bougies blindly (Gastrointest Endosc 2000;51:460–462). In most cases (85–93%) of peptic oesophageal, dilatation gives good symptom relief. However, when dilatations fail, recurrent strictures may be treated with triamcinolone injection (Gastrointest Endosc 1995; 41:596–598). Most trials have been carried out using a standard sclerotherapy needle and injecting the stricture with four 1-mL aliquots of 10 mg/mL triamcinolone in a four-quadrant pattern, for a total of 40 mg. For strictures which recur in spite of local steroids, temporary stenting using removable oesophageal stents is an alternative treatment strategy. So, which answer is correct? I would say, A ! At the time, I couldn't see the sense in scoping the patient. Indeed, this turned out to be the case! My endoscopy didn't affect management in any way. The patient was discharged a week later for psychiatric follow up only. |
Categories
All
|