|
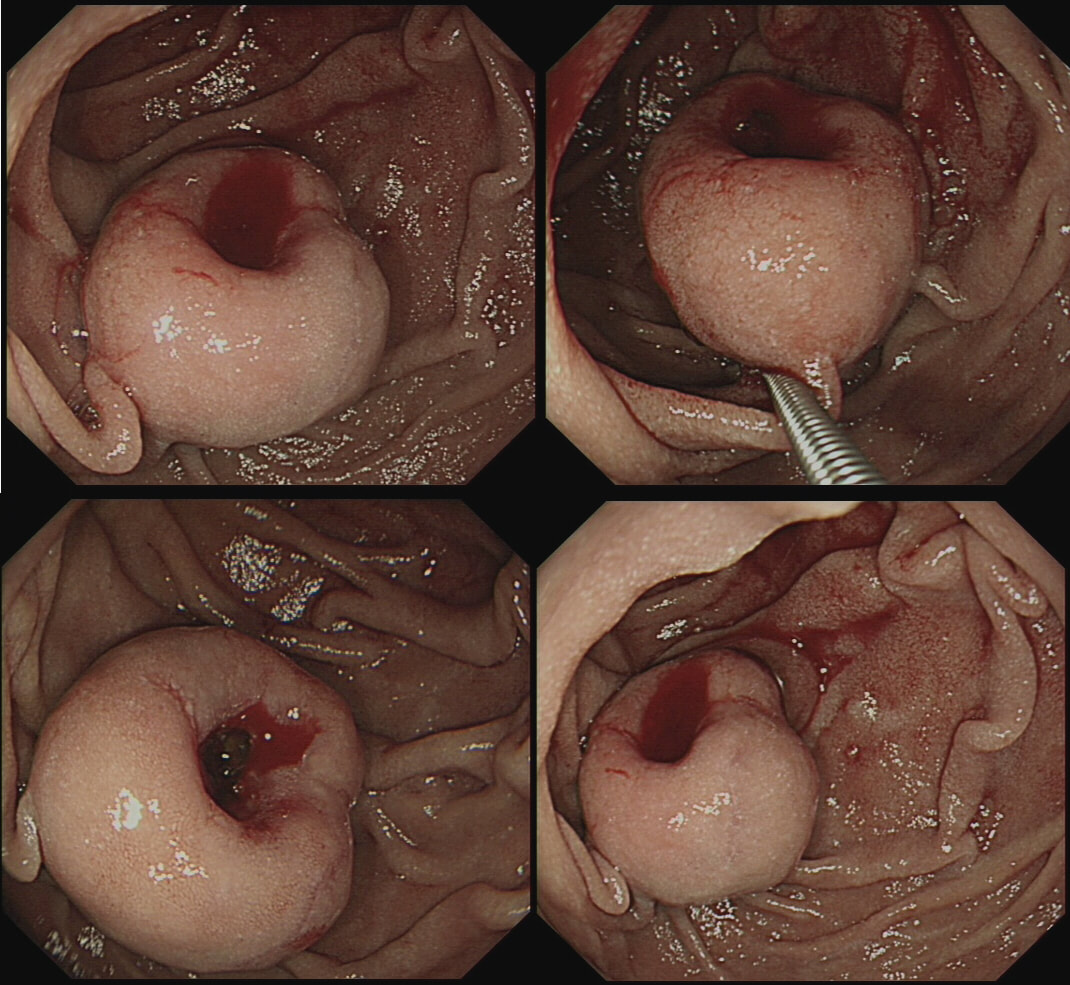
This duodenal lesion was an incidental finding in a 55 year old patient with dyspepsia.
WHAT IS THE LIKELY DIAGNOSIS?
■ GIST
Could be but something else is more likely
■ Leiomyoma
These are rare in the duodenum!
■ NET
Yes, most duodenal NET's are umbilicated!
■ Adenoma
Duodenal adenomas are often IIc lesion but not like this!
■ Carcinoma
Too pretty to be malignant!
explanation
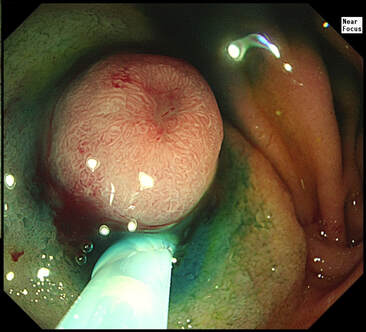
Umbilicated lesions in the duodenum are usually NET's. Even when the NET is as small as 7-8mm they will usually start to develop a central dimple as in the example below !
Ampullary NET's have a far worse prognosis than NET's situated elsewhere in the duodenum and are therefore first considered for a surgical resection. However, a small non-functioning, non-ampullary NET's may be considered for endoscopic resection.
I don't think that I was thinking entirely clearly when I accepted the referral from the Neuroendocrine 'multi-disciplinary team' for an attempt at endoscopic resection. The lesion is about 2cm and I quoted a 1:10 risk of requiring an emergency surgery in case of a perforation. This was probably an underestimate because NET's develop in the submucosa and you almost have to scrape them off the muscle propria layer which is VERY thin in the duodenum. Furthermore, I think that a small unrecognised 'micro-perforation' in the stomach is probably often 'sorted out' by a timely intervention by our great friend - the omentum! The duodenum on the other hand is retro-peritoneal and bathing in pancreatic juices. After 12 hours, that 1mm perforation will be 1 inch across and the patient will be in a desperate state. For this reason, if you do undertake duodenal resections you should be backed up with a 24-hour/day 364 day/year specialised pancreatic emergency surgery service. It's no good having an breast surgeon trying to patch things up! Now being an older and more experienced endoscopist, I believe that a far more sensible cut-off for endoscopic resection of a duodenal NET is probably 10-15mm. Personally, in an old person with comorbidities, who are unlikely to survive an emergency laparotomy, I would decline if I thought that the risk of emergency surgery was <1:100. Of course the NET could grow but is unlikely to turn malignant and kill an 85 year old patient with a previous myocardial infarction and dodgy kidney function. Particularly if the lesion is 'WHO grade is 1' only ! Of course Rembackens Resection Rule #15 applies: "A good endoscopist knows when to resect and a great endoscopist when to reassure! Also known as "Disengage if there is Disease". |
Categories
All
|