|
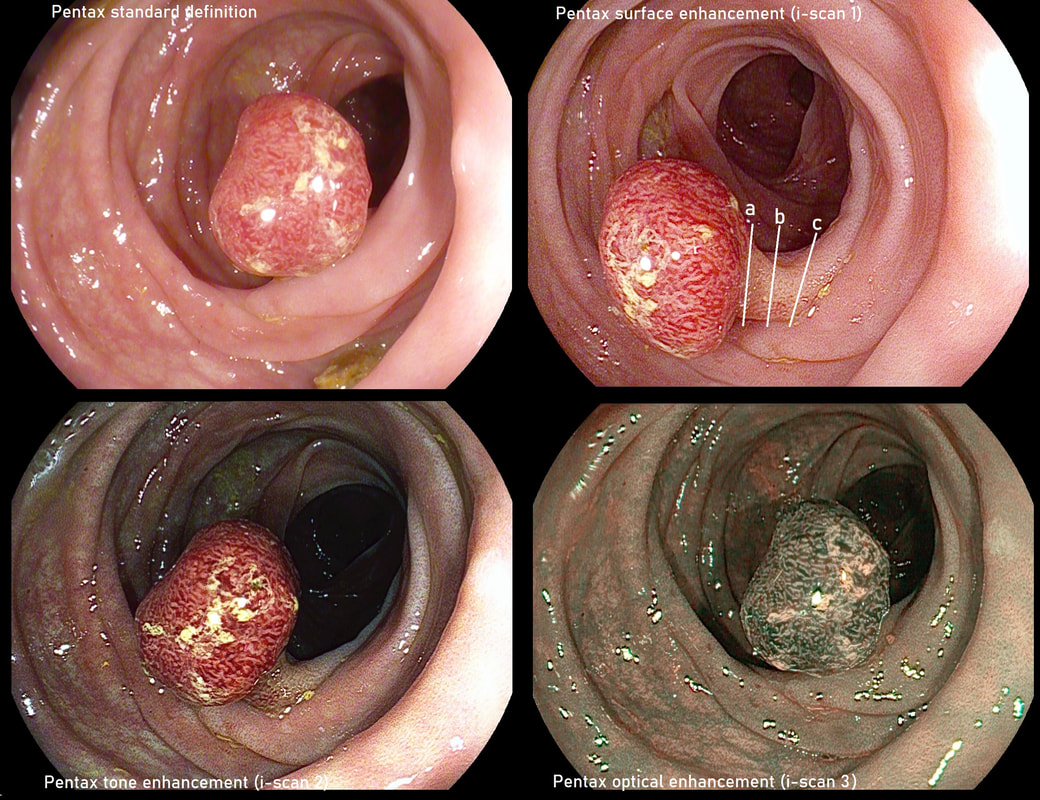
A small colonic TA+LGD as visualised by Pentax's 4 different optical modes. WHAT SIZE SNARE TO USE? a) 10mm b) 15mm c) 20mm d) 25mm WHERE TO PLACE THE SNARE (top right image)? a) at 'a' b) at 'b' c) at 'c' explanation
Even with a small polypectomy such as this there are things to discuss. FIRST, select a snare which fits nicely around the polyp. In this case, a 10mm snare is probably optimal. A snare which fits snuggly, is less likely to capture a fold of mucosa somewhere behind the polyp. In this case, you could probably see if this is happening but particularly in an angulated and spastic sigmoid, capturing too much mucosa can be an issue. Of course, if I have already used a larger snare elsewhere in the colon, I would consider using that snare again. I do try to keep costs down if possible 😳 ! SECOND, place the snare in the middle of the stalk (at b). Giving a small amount of stalk for the pathologists to confirm that the polyp has been completely removed will avoid a subsequent 'site-check'. Conversely, placing the snare too close to the base may cause two problems: a) more heat damage is imparted onto the nearby colonic wall and b) you no longer have a stump to re-capture if there is bleeding. Which leads me on to the THIRD point; 'haemostasis'. Bleeding is the main concern for us all when we do polypectomy, EMR and even ESD. My approach is as follows: ■ Anticipate bleeding! It's more likely with large polyps or polyps with thick stalks. Consider what you will do if there is bleeding. For a stalked polyp, the best option is to re-snare the polyp. For a large sessile polyp, a haemostatic forceps is usually the best bet. Ask your assistant to have the forceps immediately available (still in it's sterile packaging). By the way, I usually use a 'hot biopsy forceps' because they cost £10 compared to the £200 for a fancy haemostatic forceps. ■ Prevention. Most admit that I never place a clip on the stalk before cutting it. This is because the current can easily travel down the clips tail and cause a burn at some unexpected place. However, I often pre-inject a thick stalks and large pedunculated polyps with dilute adrenaline. It will buy me a valuable minute of 'gentle oozing' from the vessel before the floodgates open. At ESD, you will of course coagulate the vessels as they appear in your dissection field. A large sessile 4cm polyp can be removed by single fragment EMR (there are snares large enough) but you will of course have to deal with several bleeding vessels once the polyp has come off. Of course, at ESD you can deal with the vessels one-by-one and this may be preferable than going for the 'quick option' of an EMR. Under the heading "Prevention", I should also mention that I advice my assistant on how many seconds I think it will take to cut the polyp. I also tell them that once they see the stalk being cut by the snare, they should ease off and stop closing the handle. The 'inertia' in the system will cut the rest of the polyp at the appropriate speed. After all, the vessels are in the CENTRE of the stalk and it's the last few seconds of cutting which deals with them! You don't want to rush this bit!!! For this reason, I am not a fan of 'pre-coagulating' the stalk by pressing on the blue pedal first. This cooks the harmless outside of the stalk but leaves the important centre intact. If anything one should do the opposite! Actually, with modern diathermy you don't need to concern yourself as the clever machines deliver mainly 'cut' at the beginning (when the resistance in the electrical circuit is greater) and then moves to short pulses of 'coagulation' and 'pause' (to allow tissues to cool down) as the electrical resistance drops as the stalk is cut. ■ Clipping. This deserves it's own 'heading'. I almost always place clips unless it's cold snaring a small polyp in a patient who is not taking blood thinners. Of course, I work in a part of the world when I don't need to worry about whether the patient can actually afford the clips 🙂 . When you feel exhausted after a 60 minute resection, it's easy to leave the clips out. It would be a mistake! Clipping reduces the risk of both late bleeding, the post-polypectomy syndrome and late perforations! |
Categories
All
|